Types of Airway Management Devices
Safe and effective airway management is a central aspect of healthcare that requires clinical expertise in many different situations. Whether a patient is in for a routine operation or attending the hospital in a life-threatening emergency, medical professionals need airway management training and easy access to the right equipment to maintain a patient's airway patency. The core purpose of airway management is to facilitate the continuous transportation of oxygen to a patient's lungs. This is central to all areas of medicine, including emergency care, surgical operations, intensive care, general wards, and much more.

Steroplast has been a trusted emergency services supplier for over 25 years, so we have the knowledge and expertise to help unpack this essential component of medical care. This article will discuss the most common types of airway management devices relied on throughout healthcare, including a range of supraglottic devices, definitive airway management devices, and ventilation equipment. We'll take you through what they are, how they are used, and the situations they are best suited to, covering essential items on a medical airway management equipment list.
The Anatomy of the Airway
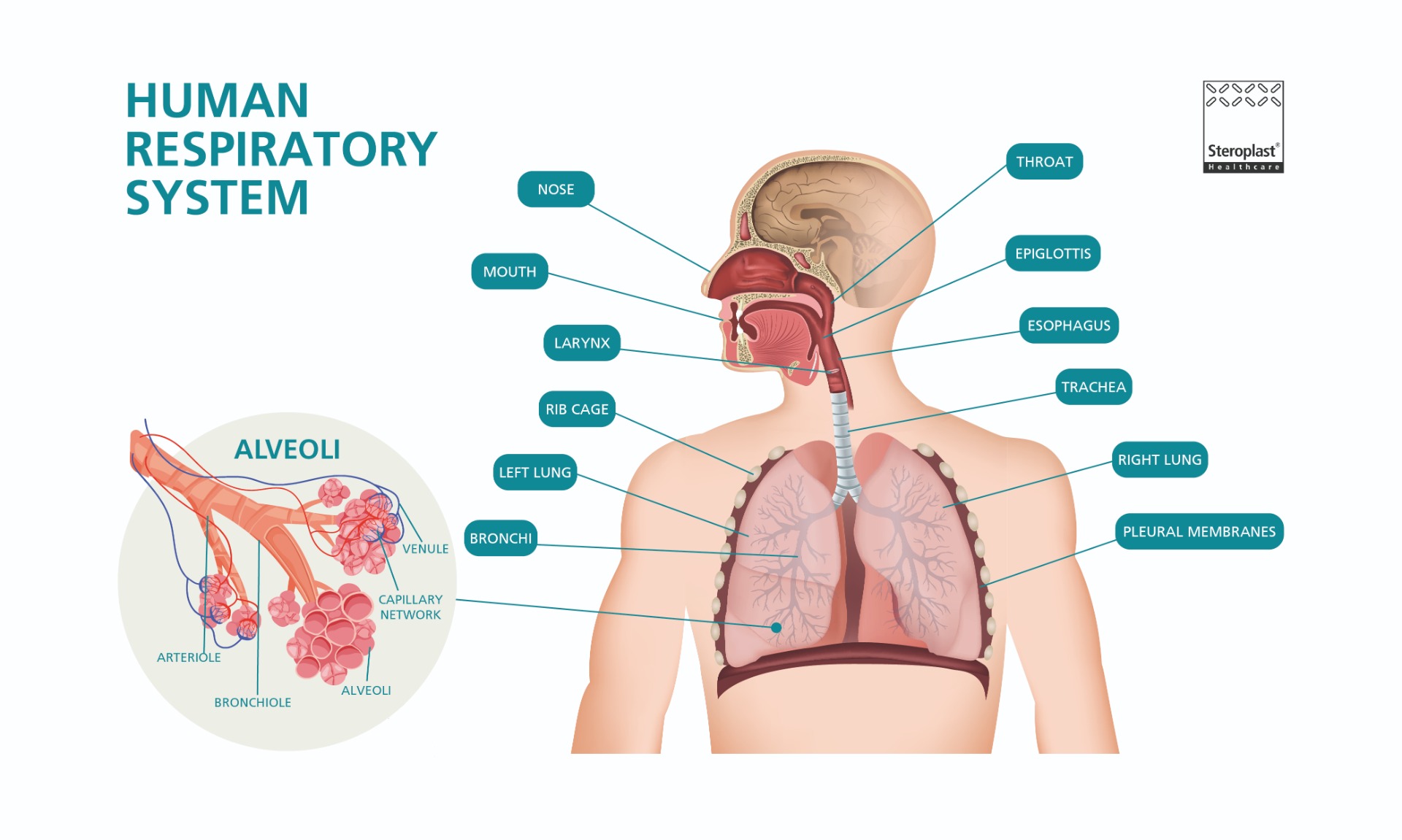
The proper functioning of your airway is essential to survival, meaning that the airway anatomy is a vital part of the human body. Before we take you through the different types of airway management devices used to ensure oxygen can reach the lungs when the airway is compromised, let's unpack the structure of the airway anatomy, also called the respiratory system.
The Upper Airway
Broken down into the nose, mouth, and throat, the upper airway is oxygen's entry point into the respiratory system. Obstruction or damage to these structures can rapidly lead to unconsciousness or death.
| Nose (Nasopharynx) | The primary airway that most conscious adults use to breathe naturally. |
|---|---|
| Mouth | The alternate airway to the nose, the mouth is critical in emergency airway management situations. |
| Throat (Oropharynx/Larynx) | The oropharynx is the area at the back of the mouth behind the tongue, connecting the nose and larynx. The epiglottis (which covers the opening of the trachea to prevent swallowed food from entering the lower airway) separates the oropharynx and the larynx (voice box). |
The Lower Airway
Covering everything below the larynx, the lower airway comprises various tubes that transfer air into structures inside the lungs that facilitate respiration (the exchange of oxygen and carbon dioxide).
| Trachea | Also referred to as the windpipe, the trachea is the hollow tube that passes air down into the lower airways. It is strengthened and supported by cartilage rings. It moistens and warms air as it travels down into the lungs. |
|---|---|
| Lungs | Both the right and left lungs are located in the thoracic cavity in the chest. They facilitate inhalation and exhalation by expanding and contracting, bringing fresh oxygen in and removing carbon dioxide and other waste gases. This is facilitated by the diaphragm muscle and the external intercostal muscles between the ribs. |
| Bronchial Tree (Bronchi and Bronchioles) | Bronchi are hollow tubes that carry oxygen from the trachea, subdividing into smaller bronchi to distribute air into both lungs, branching off into smaller bronchioles that interact with alveoli. |
| Alveoli | These are the millions of thin-walled sacs located deep inside the lungs, surrounded by a complex network of capillaries, forming the body's air-blood barrier. Bronchioles transfer air to the alveoli, which then exchange gases with the blood in the capillaries. This allows for efficient respiration and maintenance of the body’s oxygen levels, removing carbon dioxide from the respiratory system via exhalation. |
Simplify Workplace First Aid
Interactive Online Guide & Downloadable Brochure
Simplify Workplace First Aid
Interactive Online Guide & Downloadable Brochure
Choose the format that works for you: check out our Workplace First Aid Interactive Online Guide or download our 2-in-1 Workplace First Aid & Advanced Life Support Buyers Guide as an easy-to-save PDF. Both include a self-assessment, product details, and comprehensive training and support.
Understanding Airway Management
Airway management incorporates the assessment, planning, and necessary medical procedures required to maintain or restore a patient's breathing. It is fundamental to emergency care, and effective airway management is an essential skill for medical professionals throughout healthcare.
The primary aims of airway management are to:
- Establish airway patency (being open and unobstructed)
- Ensure ventilation of the lungs
- Protect from pulmonary soiling or aspiration (materials entering the lungs such as liquid, food, or blood)
Successful airway management should ensure gas exchange and protect the lungs from injury to allow for medical treatment. Safe airway management relies on the effective, reliable use of appropriate equipment, often requiring a combination of different types of airway management devices.
When is airway management required?
Improper airway functioning can occur in a wide range of situations and requires a quick response. Some of the most common indications for the implementation of airway management procedures include:
- Respiratory failure
- Active choking
- Penetrating trauma
- Reduced level of consciousness
- Rapid changes in mental state
- During surgical procedures requiring anaesthesia
Clinicians should form an airway management strategy and factor in backup plans to ensure airway management is safe and successful. Correct knowledge, skill and attitudes are essential throughout healthcare to ensure the safe use of items found on a standard airway management equipment list.
Advancements in airway management devices and practices are continuously evolving, with new technologies or improvements being made to improve the safety and effectiveness of airway management across the medical sector.
Exploring the Different Types of Airway Management Devices Used in Healthcare
Supraglottic Airway Devices (SADs)
Supraglottic airway management devices, sometimes shortened to supraglottic airways or SADs, are a class of devices used to open or maintain a patient's airway. The term ‘supraglottic’ means above the larynx or glottis, meaning a supraglottic airway acts above the level of the voice box. SADs facilitate oxygenation, ventilation, and administration of anaesthetic gases without requiring endotracheal intubation.
SADs are often used in situations where intubation is not necessary or feasible or when a clinician needs to secure the airway quickly. The largest ever study into airway management, the NAP4 report titled ‘Major Complications of Airway Management in the United Kingdom’, argues that SADs ‘have a vital role in difficult airway management’ including:
- The primary airway rescue device out of hospital settings.
- The rescue of the airway after the failure of other airway devices including mask ventilation or tracheal intubation.
- To assist fibreoptic intubation.
There are various types of supraglottic airway devices used in medical care. We break down the most common and widely trusted SAD devices included on a standard airway management equipment list below.
Click to expand:
The first laryngeal mask airway was introduced in 1989 and quickly adopted as a key device for routine and emergency airway management. A traditional LMA consists of a tube with an inflatable cuff (balloon) inserted into the throat. The cuff inflates to form a seal around the opening that connects the pharynx and larynx (laryngeal inlet), allowing continuous ventilation.
Since the first LMA device's patent expired, LMAs have seen major improvements in design and functionality. The NAP4 report notes that these newer LMA devices, including the i-gel Supraglottic Airway we stock, are specifically designed to increase safety and efficacy.
Devices like the i-gel don’t rely on the inflatable cuff mechanism to form a seal, with the rim of the mask designed to conform to the shape of the larynx instead, it can adapt its form based on the patient’s unique anatomy to ensure an airtight seal. The i-gel’s tube incorporates a breathing tube and a drain tube, making it possible to intubate through the breathing tube and insert a gastric tube through the drainage tube if required.
The comprehensive NAP4 airway management report argues that second-generation designs of LMAs, like the i-gel offer the following benefits in airway management:
- Improved pharyngeal seal enabling controlled ventilation at higher airway pressures (and hence in a wider range of patients and clinical situations)
- Increased oesophageal seal, which lessens the likelihood of regurgitant fluids entering the pharynx and leading to aspiration
- A drain tube which lies over the top of the oesophagus when the SAD is correctly positioned. This may be used to assist insertion, confirm correct device positioning, enable access to the stomach, alert the user to the presence of regurgitation and enable gastric contents to bypass the oropharynx and exit the patient safely.
Intubating laryngeal mask airways are a variation of the more widely used LMA devices. ILMAs, such as a Fastrach LMA, feature a built-in guide for an endotracheal tube which allows for blind intubation, most often used in scenarios where airway management is difficult.
Oropharyngeal airways (OPAs), also called Guedel airways, are simple curved hollow tubes used to maintain the patient's airway by preventing the tongue from obstructing the top of the throat. These small devices are first lubricated with sterile water-soluble lubricating jelly such as OptiLube Jelly. They are then inserted into the mouth upside down and twisted into position. They should only be used on highly unresponsive patients who are unable to maintain their airways independently, as they can cause conscious patients to gag and vomit and can lead to aspiration if used incorrectly.
If a patient is responsive and, therefore, an OPA is unsuitable, clinicians may opt to use a nasopharyngeal airway (NPA), a narrow tube made from soft rubber or plastic. An NPA (also called a nasal trumpet) is inserted into a patient’s nostril to pass through the nose and reach the pharynx, bypassing any obstruction from the tongue. Though many patients report that insertion of an NPA is unpleasant, they are more easily tolerated than OPAs, especially in the event of a semiconscious patient or tightly clenched jaw.
Both OPAs and NPAs are relatively easy to insert safely and can be used effectively with bag-mask ventilation. Neither of these devices prevents aspiration, so the patient should be constantly monitored. OPA and NPA devices are best used as short-term airway management solutions.
The laryngeal tube (LT) device comprises two airway tubes bonded together with two low-pressure cuffs (balloons). Inserted blindly, one cuff sits above the glottis, and the other cuff acts as an oesophagal blocker which is designed to prevent aspiration. The airway tubes' ventilation outlets are located between the cuffs to facilitate ventilation of the lungs.
There are several versions of the LT airway, with disposable or reusable products available. LTs are a good alternative when endotracheal intubation or LMAs are not viable or unsuccessful and are commonly used during anaesthesia and cardiopulmonary resuscitation to facilitate mechanical lung ventilation.
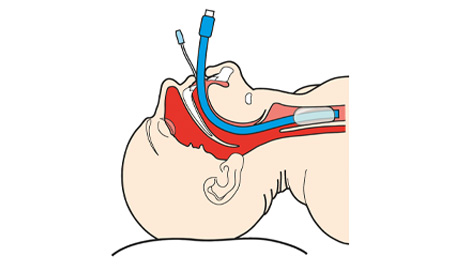
It’s important to note that a laryngeal tube airway requires regular monitoring and readjustment of its position to ensure the airway remains clear and should be fitted by a trained, experienced professional.
The oesophageal-tracheal Combitube is a double-cuff (balloon) device similar to the laryngeal tube. However, it can be inserted into the trachea or oesophagus to be used either for ventilation or to prevent aspiration. Combitubes should only be used on unresponsive, apneic, or pulseless patients and can be used effectively in out-of-hospital emergency situations by an experienced, trained medical professional. These devices are widely considered to be good backup airway management solutions when intubation or ventilation efforts have been unsuccessful.
Endotracheal Intubation and Tracheostomy
Difficult airway scenarios often require more definitive airway management methods than most supraglottic devices can provide. Two of the key types of airway management devices used in routine, surgical and emergency care facilitate intubation or tracheostomy procedures. We’ll take you through the use of endotracheal tubes and related intubation equipment and explain some cases in which a tracheostomy is required to bypass upper airway obstructions to ensure airway patency.
Click to expand:
The intubation process refers to inserting an endotracheal tube into the trachea to facilitate respiration. Intubation is often necessary when a patient’s airway is damaged or blocked, or they are unable to breathe spontaneously. According to the NAP4 report, approximately 1 in 800 patients attending the A&E will require intubation and the induction of anaesthesia as part of their emergency care, equating to approximately 20,000 UK patients each year in A&E alone.
Opting for endotracheal intubation as an emergency airway management strategy is often required when treating patients with the following conditions:
- Obstruction of the airway
- Sudden cardiac arrest
- Apnea or respiratory failure
- Trauma to the neck, chest or abdomen
- Loss of consciousness (when it affects the patient’s airway control)
Intubation is also common practice in surgical settings. When a patient undergoes surgery and needs to be anaesthetised, they cannot breathe on their own, so the endotracheal tube is fitted to a respiratory machine to facilitate respiration, oxygenation and the transfer of gasses. The NAP4 report argues that ‘there will always be an irreducible requirement for tracheal intubation during anaesthesia’ as well as in emergency care.
Airway Management Equipment List for a Successful Intubation Procedure
Safe, successful intubation requires the use of various types of airway management devices to ensure correct placement.
A flexible plastic tube fitted with an inflatable cuff to seal the trachea and prevent aspiration once inserted.
Bougies are thin, flexible devices that aid the insertion of an endotracheal tube. Bougies are especially advantageous in difficult airway scenarios.
A visual aid for intubation that features a handle, a lightbulb and a dull blade to help clinicians guide the endotracheal tube.
Often placed over the nose and mouth before a patient is intubated to provide extra oxygen.
ETCO2 detectors are tools that are attached to the endotracheal tube to monitor End Tidal CO2 level of the patient’s breath. This additional safety measure for intubation changes colour when CO2 levels are too high, alerting healthcare providers to respond.
In some cases, a tracheostomy may be required to bypass the upper airway and ensure oxygen reaches the lungs without obstruction. The tracheotomy procedure is performed under general anaesthesia and involves creating an opening via an incision in the patient’s throat, through into the trachea. A tracheostomy tube is inserted into the opening to provide an airway.
In most cases, a tracheostomy is a short-term airway management solution. However, patients in an ICU may be connected to a ventilator via a tracheostomy tube if they are expected to remain unconscious for extended periods. Tracheostomy tubes require regular assessment and cleaning to maintain the correct position and prevent infection.
Non-Invasive Devices and Ventilation Equipment
Click to expand:
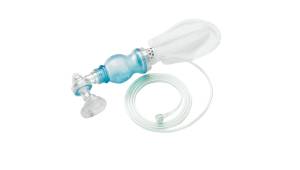
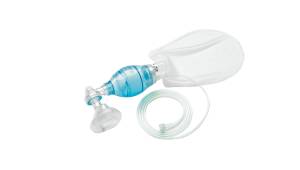
Bag-valve-masks are common types of airway management devices used throughout emergency and hospital care. They feature a face mask with a one-way valve fitted with a self-inflating bag to facilitate manual resuscitation and assist a patient’s breathing.
Steroplast stocks a range of bag-valve-masks and resuscitators to suit a variety of patient needs:
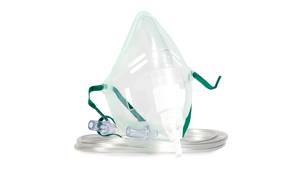
Nasal cannulae and oxygen masks are often used to deliver supplemental oxygen therapy when patients require it, through either the mouth or nose. While these types of airway management devices do not directly open or maintain an airway, they are used to support patients who experience respiratory problems.
Steroplast supplies UK hospitals and care facilities with premium oxygen therapy equipment, check out our range:
Other Essential Items for an Airway Management Equipment List
Now we have covered the types of airway management devices most commonly used in healthcare, it’s essential to consider other pieces of medical equipment and accessories that support safe airway management.
Monitors
Click to expand:
A capnograph is an electronic device that measures the CO2 concentration of gases in a patient's airway, giving real-time information to healthcare providers. Capnography monitoring is mandatory for intubated patients undergoing surgery in theatre, and a capnograph is used to monitor the efficacy of an artificial airway device in a range of situations, including patients under sedation, those with a tracheostomy or endotracheal tube fitted, those in ICU, and is also useful when weaning patients off ventilatory support and for patients who are not intubated.
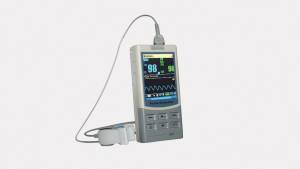
A pulse oximeter is a non-invasive device that measures the oxygen saturation in a patient's blood. They have a wide range of applications throughout healthcare and can play a critical role in airway management. Pulse oximetry can help to detect respiratory failure when an artificial airway device is in use, and can also support the triage and diagnosis of patients with compromised airways by identifying those suffering from hypoxemia.
Steroplast stocks a selection of professional grade pulse oximeters.
The assessment and continuous monitoring of a patient’s heart rate, blood pressure and body temperature while airway management devices are in use supports clinicians in ensuring airway patency and full respiratory function is maintained.
Other Airway Management Tools and Accessories
Click to expand:
Several types of airway management devices, including endotracheal tubes, bougies, nasopharyngeal and oropharyngeal airways require lubrication to aid insertion into a patient’s airway. We stock OptiLube sterile lubricating jelly, which is water soluble, making it ideal for airway management.
Suction is commonplace in surgical settings as well as emergency care. Effective suction is critical to many types of airway management, used to maintain airway patency by removing liquids from the trachea or mouth.
Many hospital setups benefit from the allocation of a dedicated moveable vessel that contains all specialist types of airway management devices in one place. A dedicated, well-organised trolley is an essential part of a comprehensive airway management equipment list, ensuring quick access to all devices required.
Important Take Aways for Airway Management Success
A huge range of airway management devices are available for many different applications and scenarios. Having the right skills, attitude, and equipment available is critical to a successful airway management strategy, and selecting the right device requires comprehensive training and experience to ensure positive patient outcomes.
The airway management field is subject to continuous developments and advancements in technology, equipment, training, and procedures which will continue to influence healthcare and improve the quality of care for years to come. This means that regular and up-to-date training must incorporate traditional and new methods for healthcare staff to ensure they are equipped with the knowledge and skills to decide on and implement the most appropriate airway strategies and respond accordingly.
It’s critical that clinicians have access to the tools included on a comprehensive airway management equipment list, including monitoring devices and airway management accessories, to ensure airway management is successful and safe.
On top of this, clinicians and medical staff need to prioritise good organisation of airway management equipment and implement thorough cleaning and sterilisation practices to maintain optimal hygiene and infection control.
If you have any questions regarding the airway management equipment we stock, don’t hesitate to get in touch and speak with a member of our team today.
Steroplast is a leading medical supplier to emergency services and hospitals across the UK. If you're keen to learn more about medical equipment, and healthcare best practices, and gain expert tips and insights, check out the following articles on our comprehensive Knowledge Base:
Please enter your details into the form below along with any questions or comments and a member of our team will be happy to provide you with more information:
Safe and effective airway management is a central aspect of healthcare that requires clinical expertise in many different situations. Whether a patient is in for a routine operation or attending the hospital in a life-threatening emergency, medical professionals need airway management training and easy access to the right equipment to maintain a patient's airway patency. The core purpose of airway management is to facilitate the continuous transportation of oxygen to a patient's lungs. This is central to all areas of medicine, including emergency care, surgical operations, intensive care, general wards, and much more.

Steroplast has been a trusted NHS and emergency services supplier for over 25 years, so we have the knowledge and expertise to help unpack this essential component of medical care. This article will discuss the most common types of airway management devices relied on throughout healthcare, including a range of supraglottic devices, definitive airway management devices, and ventilation equipment. We'll take you through what they are, how they are used, and the situations they are best suited to, covering essential items on a medical airway management equipment list.
The Anatomy of the Airway
The proper functioning of your airway is essential to survival, meaning that the airway anatomy is a vital part of the human body. Before we take you through the different types of airway management devices used to ensure oxygen can reach the lungs when the airway is compromised, let's unpack the structure of the airway anatomy, also called the respiratory system.
The Upper Airway
Broken down into the nose, mouth, and throat, the upper airway is oxygen's entry point into the respiratory system. Obstruction or damage to these structures can rapidly lead to unconsciousness or death.
| Nose (Nasopharynx) | The primary airway that most conscious adults use to breathe naturally. |
|---|---|
| Mouth | The alternate airway to the nose, the mouth is critical in emergency airway management situations. |
| Throat (Oropharynx/Larynx) | The oropharynx is the area at the back of the mouth behind the tongue, connecting the nose and larynx. The epiglottis (which covers the opening of the trachea to prevent swallowed food from entering the lower airway) separates the oropharynx and the larynx (voice box). |
The Lower Airway
Covering everything below the larynx, the lower airway comprises various tubes that transfer air into structures inside the lungs that facilitate respiration (the exchange of oxygen and carbon dioxide).
| Trachea | Also referred to as the windpipe, the trachea is the hollow tube that passes air down into the lower airways. It is strengthened and supported by cartilage rings. It moistens and warms air as it travels down into the lungs. |
|---|---|
| Lungs | Both the right and left lungs are located in the thoracic cavity in the chest. They facilitate inhalation and exhalation by expanding and contracting, bringing fresh oxygen in and removing carbon dioxide and other waste gases. This is facilitated by the diaphragm muscle and the external intercostal muscles between the ribs. |
| Bronchial Tree (Bronchi and Bronchioles) | Bronchi are hollow tubes that carry oxygen from the trachea, subdividing into smaller bronchi to distribute air into both lungs, branching off into smaller bronchioles that interact with alveoli. |
| Alveoli | These are the millions of thin-walled sacs located deep inside the lungs, surrounded by a complex network of capillaries, forming the body's air-blood barrier. Bronchioles transfer air to the alveoli, which then exchange gases with the blood in the capillaries. This allows for efficient respiration and maintenance of the body’s oxygen levels, removing carbon dioxide from the respiratory system via exhalation. |
Understanding Airway Management
Airway management incorporates the assessment, planning, and necessary medical procedures required to maintain or restore a patient's breathing. It is fundamental to emergency care, and effective airway management is an essential skill for medical professionals throughout healthcare.
The primary aims of airway management are to:
- Establish airway patency (being open and unobstructed)
- Ensure ventilation of the lungs
- Protect from pulmonary soiling or aspiration (materials entering the lungs such as liquid, food, or blood)
Successful airway management should ensure gas exchange and protect the lungs from injury to allow for medical treatment. Safe airway management relies on the effective, reliable use of appropriate equipment, often requiring a combination of different types of airway management devices.
When is airway management required?
Improper airway functioning can occur in a wide range of situations and requires a quick response. Some of the most common indications for the implementation of airway management procedures include:
- Respiratory failure
- Active choking
- Penetrating trauma
- Reduced level of consciousness
- Rapid changes in mental state
- During surgical procedures requiring anaesthesia
Clinicians should form an airway management strategy and factor in backup plans to ensure airway management is safe and successful. Correct knowledge, skill and attitudes are essential throughout healthcare to ensure the safe use of items found on a standard airway management equipment list.
Advancements in airway management devices and practices are continuously evolving, with new technologies or improvements being made to improve the safety and effectiveness of airway management across the medical sector.
Exploring the Different Types of Airway Management Devices Used in Healthcare
Supraglottic Airway Devices (SADs)
Supraglottic airway management devices, sometimes shortened to supraglottic airways or SADs, are a class of devices used to open or maintain a patient's airway. The term ‘supraglottic’ means above the larynx or glottis, meaning a supraglottic airway acts above the level of the voice box. SADs facilitate oxygenation, ventilation, and administration of anaesthetic gases without requiring endotracheal intubation.
SADs are often used in situations where intubation is not necessary or feasible or when a clinician needs to secure the airway quickly. The largest ever study into airway management, the NAP4 report titled ‘Major Complications of Airway Management in the United Kingdom’, argues that SADs ‘have a vital role in difficult airway management’ including:
- The primary airway rescue device out of hospital settings.
- The rescue of the airway after the failure of other airway devices including mask ventilation or tracheal intubation.
- To assist fibreoptic intubation.
There are various types of supraglottic airway devices used in medical care. We break down the most common and widely trusted SAD devices included on a standard airway management equipment list below.
Click to expand:
The first laryngeal mask airway was introduced in 1989 and quickly adopted as a key device for routine and emergency airway management. A traditional LMA consists of a tube with an inflatable cuff (balloon) inserted into the throat. The cuff inflates to form a seal around the opening that connects the pharynx and larynx (laryngeal inlet), allowing continuous ventilation.
Since the first LMA device's patent expired, LMAs have seen major improvements in design and functionality. The NAP4 report notes that these newer LMA devices, including the i-gel Supraglottic Airway we stock, are specifically designed to increase safety and efficacy.
Devices like the i-gel don’t rely on the inflatable cuff mechanism to form a seal, with the rim of the mask designed to conform to the shape of the larynx instead, it can adapt its form based on the patient’s unique anatomy to ensure an airtight seal. The i-gel’s tube incorporates a breathing tube and a drain tube, making it possible to intubate through the breathing tube and insert a gastric tube through the drainage tube if required.
The comprehensive NAP4 airway management report argues that second-generation designs of LMAs, like the i-gel offer the following benefits in airway management:
- Improved pharyngeal seal enabling controlled ventilation at higher airway pressures (and hence in a wider range of patients and clinical situations)
- Increased oesophageal seal, which lessens the likelihood of regurgitant fluids entering the pharynx and leading to aspiration
- A drain tube which lies over the top of the oesophagus when the SAD is correctly positioned. This may be used to assist insertion, confirm correct device positioning, enable access to the stomach, alert the user to the presence of regurgitation and enable gastric contents to bypass the oropharynx and exit the patient safely.
Oropharyngeal airways (OPAs), also called Guedel airways, are simple curved hollow tubes used to maintain the patient's airway by preventing the tongue from obstructing the top of the throat. These small devices are first lubricated with sterile water-soluble lubricating jelly such as OptiLube Jelly. They are then inserted into the mouth upside down and twisted into position. They should only be used on highly unresponsive patients who are unable to maintain their airways independently, as they can cause conscious patients to gag and vomit and can lead to aspiration if used incorrectly.
If a patient is responsive and, therefore, an OPA is unsuitable, clinicians may opt to use a nasopharyngeal airway (NPA), a narrow tube made from soft rubber or plastic. An NPA (also called a nasal trumpet) is inserted into a patient’s nostril to pass through the nose and reach the pharynx, bypassing any obstruction from the tongue. Though many patients report that insertion of an NPA is unpleasant, they are more easily tolerated than OPAs, especially in the event of a semiconscious patient or tightly clenched jaw.
Both OPAs and NPAs are relatively easy to insert safely and can be used effectively with bag-mask ventilation. Neither of these devices prevents aspiration, so the patient should be constantly monitored. OPA and NPA devices are best used as short-term airway management solutions.
The laryngeal tube (LT) device comprises two airway tubes bonded together with two low-pressure cuffs (balloons). Inserted blindly, one cuff sits above the glottis, and the other cuff acts as an oesophagal blocker which is designed to prevent aspiration. The airway tubes' ventilation outlets are located between the cuffs to facilitate ventilation of the lungs.
There are several versions of the LT airway, with disposable or reusable products available. LTs are a good alternative when endotracheal intubation or LMAs are not viable or unsuccessful and are commonly used during anaesthesia and cardiopulmonary resuscitation to facilitate mechanical lung ventilation.

It’s important to note that a laryngeal tube airway requires regular monitoring and readjustment of its position to ensure the airway remains clear and should be fitted by a trained, experienced professional.
The oesophageal-tracheal Combitube is a double-cuff (balloon) device similar to the laryngeal tube. However, it can be inserted into the trachea or oesophagus to be used either for ventilation or to prevent aspiration. Combitubes should only be used on unresponsive, apneic, or pulseless patients and can be used effectively in out-of-hospital emergency situations by an experienced, trained medical professional. These devices are widely considered to be good backup airway management solutions when intubation or ventilation efforts have been unsuccessful.
Endotracheal Intubation and Tracheostomy
Difficult airway scenarios often require more definitive airway management methods than most supraglottic devices can provide. Two of the key types of airway management devices used in routine, surgical and emergency care facilitate intubation or tracheostomy procedures. We’ll take you through the use of endotracheal tubes and related intubation equipment and explain some cases in which a tracheostomy is required to bypass upper airway obstructions to ensure airway patency.
Click to expand:
The intubation process refers to inserting an endotracheal tube into the trachea to facilitate respiration. Intubation is often necessary when a patient’s airway is damaged or blocked, or they are unable to breathe spontaneously. According to the NAP4 report, approximately 1 in 800 patients attending the A&E will require intubation and the induction of anaesthesia as part of their emergency care, equating to approximately 20,000 UK patients each year in A&E alone.
Opting for endotracheal intubation as an emergency airway management strategy is often required when treating patients with the following conditions:
- Obstruction of the airway
- Sudden cardiac arrest
- Apnea or respiratory failure
- Trauma to the neck, chest or abdomen
- Loss of consciousness (when it affects the patient’s airway control)
Intubation is also common practice in surgical settings. When a patient undergoes surgery and needs to be anaesthetised, they cannot breathe on their own, so the endotracheal tube is fitted to a respiratory machine to facilitate respiration, oxygenation and the transfer of gasses. The NAP4 report argues that ‘there will always be an irreducible requirement for tracheal intubation during anaesthesia’ as well as in emergency care.
Airway Management Equipment List for a Successful Intubation Procedure
Safe, successful intubation requires the use of various types of airway management devices to ensure correct placement.
A flexible plastic tube fitted with an inflatable cuff to seal the trachea and prevent aspiration once inserted.
Bougies are thin, flexible devices that aid the insertion of an endotracheal tube. Bougies are especially advantageous in difficult airway scenarios.
A visual aid for intubation that features a handle, a lightbulb and a dull blade to help clinicians guide the endotracheal tube.
Often placed over the nose and mouth before a patient is intubated to provide extra oxygen.
ETCO2 detectors are tools that are attached to the endotracheal tube to monitor End Tidal CO2 level of the patient’s breath. This additional safety measure for intubation changes colour when CO2 levels are too high, alerting healthcare providers to respond.
In some cases, a tracheostomy may be required to bypass the upper airway and ensure oxygen reaches the lungs without obstruction. The tracheotomy procedure is performed under general anaesthesia and involves creating an opening via an incision in the patient’s throat, through into the trachea. A tracheostomy tube is inserted into the opening to provide an airway.
In most cases, a tracheostomy is a short-term airway management solution. However, patients in an ICU may be connected to a ventilator via a tracheostomy tube if they are expected to remain unconscious for extended periods. Tracheostomy tubes require regular assessment and cleaning to maintain the correct position and prevent infection.
Non-Invasive Devices and Ventilation Equipment
Click to expand:
Bag-valve-masks are common types of airway management devices used throughout emergency and hospital care. They feature a face mask with a one-way valve fitted with a self-inflating bag to facilitate manual resuscitation and assist a patient’s breathing.
Steroplast stocks a range of bag-valve-masks and resuscitators to suit a variety of patient needs:
Nasal cannulae and oxygen masks are often used to deliver supplemental oxygen therapy when patients require it, through either the mouth or nose. While these types of airway management devices do not directly open or maintain an airway, they are used to support patients who experience respiratory problems.
Steroplast supplies UK hospitals and care facilities with premium oxygen therapy equipment, check out our range:
Other Essential Items for an Airway Management Equipment List
Now we have covered the types of airway management devices most commonly used in healthcare, it’s essential to consider other pieces of medical equipment and accessories that support safe airway management.
Monitors
Click to expand:
A capnograph is an electronic device that measures the CO2 concentration of gases in a patient's airway, giving real-time information to healthcare providers. Capnography monitoring is mandatory for intubated patients undergoing surgery in theatre, and a capnograph is used to monitor the efficacy of an artificial airway device in a range of situations, including patients under sedation, those with a tracheostomy or endotracheal tube fitted, those in ICU, and is also useful when weaning patients off ventilatory support and for patients who are not intubated.
A pulse oximeter is a non-invasive device that measures the oxygen saturation in a patient's blood. They have a wide range of applications throughout healthcare and can play a critical role in airway management. Pulse oximetry can help to detect respiratory failure when an artificial airway device is in use, and can also support the triage and diagnosis of patients with compromised airways by identifying those suffering from hypoxemia.
Steroplast stocks a selection of professional grade pulse oximeters.
The assessment and continuous monitoring of a patient’s heart rate, blood pressure and body temperature while airway management devices are in use supports clinicians in ensuring airway patency and full respiratory function is maintained.
Other Airway Management Tools and Accessories
Click to expand:
Several types of airway management devices, including endotracheal tubes, bougies, nasopharyngeal and oropharyngeal airways require lubrication to aid insertion into a patient’s airway. We stock OptiLube sterile lubricating jelly, which is water soluble, making it ideal for airway management.
Suction is commonplace in surgical settings as well as emergency care. Effective suction is critical to many types of airway management, used to maintain airway patency by removing liquids from the trachea or mouth.
Many hospital setups benefit from the allocation of a dedicated moveable vessel that contains all specialist types of airway management devices in one place. A dedicated, well-organised trolley is an essential part of a comprehensive airway management equipment list, ensuring quick access to all devices required.
Important Take Aways for Airway Management Success
A huge range of airway management devices are available for many different applications and scenarios. Having the right skills, attitude, and equipment available is critical to a successful airway management strategy, and selecting the right device requires comprehensive training and experience to ensure positive patient outcomes.
The airway management field is subject to continuous developments and advancements in technology, equipment, training, and procedures which will continue to influence healthcare and improve the quality of care for years to come. This means that regular and up-to-date training must incorporate traditional and new methods for healthcare staff to ensure they are equipped with the knowledge and skills to decide on and implement the most appropriate airway strategies and respond accordingly.
It’s critical that clinicians have access to the tools included on a comprehensive airway management equipment list, including monitoring devices and airway management accessories, to ensure airway management is successful and safe.
On top of this, clinicians and medical staff need to prioritise good organisation of airway management equipment and implement thorough cleaning and sterilisation practices to maintain optimal hygiene and infection control.
If you have any questions regarding the airway management equipment we stock, don’t hesitate to get in touch and speak with a member of our team today.
Steroplast is a leading medical supplier to the NHS, emergency services and hospitals across the UK. If you're keen to learn more about medical equipment, and healthcare best practices, and gain expert tips and insights, check out the following articles on our comprehensive Knowledge Base:
Please enter your details into the form below along with any questions or comments and a member of our team will be happy to provide you with more information: